Gum Disease Linked to Greater White Matter Brain Damage in Study of 1,143 Adults
New evidence that periodontal disease is independently associated with white matter brain damage strengthens the case for systemic oral health counselling.
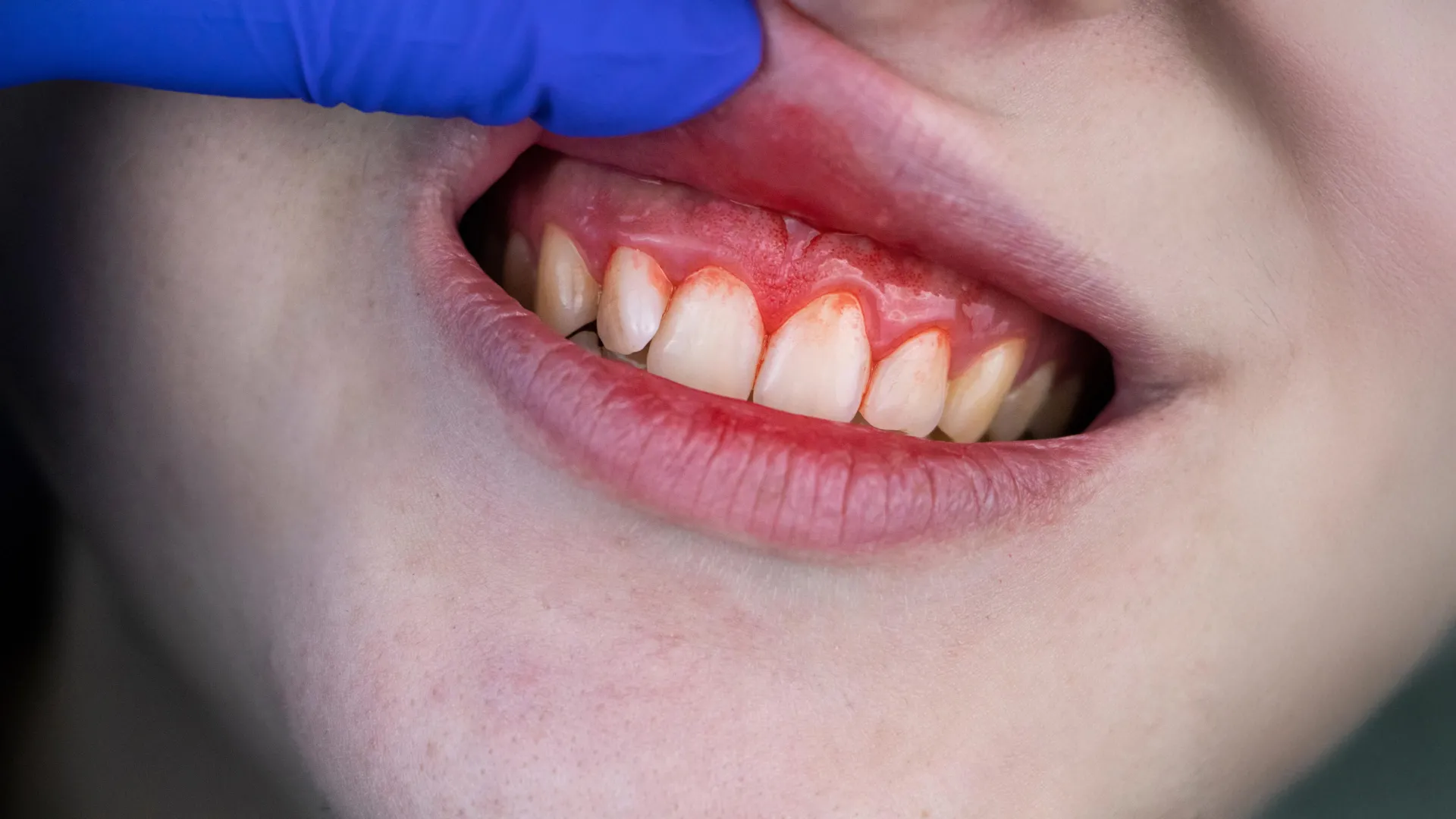
A study published October 22, 2025, in Neurology Open Access found an association between periodontal disease and higher volumes of white matter hyperintensities on brain scans. The research examined 1,143 adults with an average age of 77, of whom 800 had gum disease and 343 did not. White matter hyperintensities are bright spots visible on brain imaging that reflect areas of tissue damage; when white matter is injured, it can disrupt memory, reasoning, balance, and coordination, and it is linked to elevated stroke risk.
Participants with gum disease had a mean white matter hyperintensity volume of 2.83% of total brain volume, compared with 2.52% in those without the condition. After adjusting for age, sex, race, blood pressure, diabetes, and smoking, those with gum disease had a 56% greater likelihood of falling into the highest-volume damage group, defined as more than 21.36 cubic centimetres of affected tissue. No association was found between gum disease and cerebral microbleeds or lacunar infarcts, suggesting the relationship may be specific to white matter rather than small vessel disease broadly.
The study does not establish causation, and both dental and brain assessments were performed only once, limiting longitudinal insight. The authors, led by Souvik Sen of the University of South Carolina, note that gum disease is preventable and treatable, and that confirming this link in future research could open a route to reducing cerebral small vessel disease through oral inflammation management.